PSYCHOLOGY OF US
YOUR RESOURCE LIBRARY
CLINICAL DEPRESSION
To illustrate how horrible it was .. I would rather be in jail in a wheelchair with a body that doesn’t work than experience a severe episode of depression.
-Rob Delaney
Contents:
What Clinical Depression?
Warning signs and symptoms
Causes of Clinical Depression
Does the root cause matter? The good news.
What is Clinical Depression?
Clinical depression has been described as worse than severe injury, physical illness or grief (1). It’s been estimated that one in ten people will experience it at some point in their lives (2). However, hard as they try, doctors, neuroscientists, and psychologists have difficulty coming up with a universal definition. Is it a disorder? Is it an illness?
Why is there no universal way to define it?
In part, this is because of depression’s idiosyncratic nature. Its causes and its symptoms vary from person to person. Questions are debated yet remain unanswered. For example: Is depression a chemical imbalance? Is it a reaction to a specific situation? Is it a chemical imbalance caused by an external situation.
About the only thing that is agreed upon when it comes to a definition, is that depression is a group of physical and emotional symptoms; the most marked being a relentless malaise that permeates thought and experience and forces a seemingly inescapable sadness on its host.
Depression is not one simple emotion. Rather it is a combination of emotions – often including strong feelings of anger, fear, guilt, and shame – with sadness as its key component (3). And it affects the way we think, behave, and our bodies.
Warning Signs and Symptoms
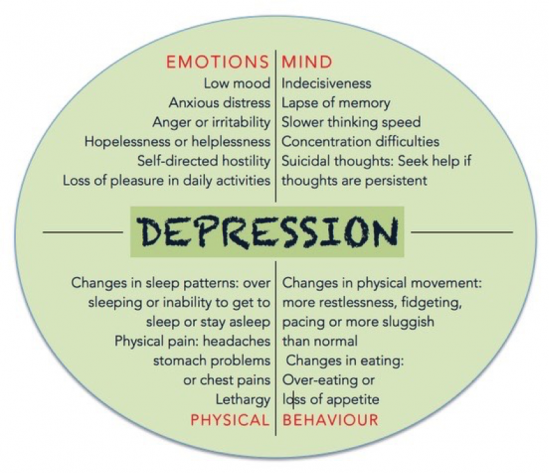
Causes of Clinical Depression
Some depression has well-known triggers. A loss of a loved one or a job, financial difficulties, trauma, and physical illness can all set off a depressive state, which can spiral into clinical depression. Not knowing why you are depressed, however, is also very common.
Unlike a broken nose or a bee sting, the root causes of depression are not always observable.
What we do know is that depression can be caused by a complex combination of environmental and biological factors (genetic propensity, for example); its underlying mechanisms are different for different people; and it happens to people from all walks of life at any time of life (4).
The most common contributors:
Trauma, abuse, or life stress in childhood. Past physical and/or emotional abuse can lead to depression later in life. Childhood stress or trauma can create negative thinking patterns, which shape our brain structure (and our ability to regulate our mood) (5). Because of early life experiences with a rejecting parent, for example, a new relationship might trigger a fear of seemingly inevitable rejection, ultimately leading to depression.
Genetics. Depression runs in families. However, no one simply inherits depression from one gene or one parent. Research suggests certain combinations of genes lead towards a propensity for depression but do not predetermine it (6).
Medications or prescription drugs. Side effects of medications may include depression. Check with your prescribing doctor if you think that this might be the case.
Hormone changes. Both men and women experience hormone shifts that affect mood. Although women are more likely to have over or underactive thyroid conditions that result in depressive symptoms, psychologist and author Jed Diamond points out that men have a number of hormonal cycles that can result in low mood (7).
Loneliness or lack of support. Social isolation or being cast out by a social group can cause emotional distress and can lead to depression.
Mood or neurodevelopment disorders such as autism. Depression can result from social isolation that occurs with such disorders.
Death or loss. Grief is a natural response to a loss of someone or something. However, such loss can trigger clinical depression.
Major events or changes in life. Negative or positive events such as stressful life events, loss of a job or a partner or graduation, moving to a new place, marriage, or retirement can all trigger depression.
Conflict. Disputes with partners, friends, family or colleagues can play a role in emotional wellbeing.
Difficulty dealing with stress. Ongoing stressors such as financial strain, negative work environment as well as the lack of resources and/or coping mechanisms can result in the onset of depression.
Powerlessness. Perceived or real inability to change our situation in positive ways. A sense of helplessness and hopelessness can increase with depression creating a depressive cycle.
Drug and alcohol abuse. Alcohol and some illegal substances have major depressive effects on the brain. But also, some people drink alcohol and take drugs to cope with feeling depressed. Nearly 30% of people with substance abuse issues have a form of depression. There is a chicken or egg question that can be asked here.

Does the root cause matter?
Depression is an umbrella term for people who have persistent low mood. All other depressive traits may be vastly different: symptoms, thinking patterns, environmental circumstances, and genetic makeups. Finding one root cause for such a disparate group of people is like looking for the root cause of all broken noses.
The good news is we don’t have to know what caused our depression to treat it.
We may not know what caused our brains propensity for depression but recent (amazing) neurological discoveries have shown us that our brains are constantly changing. Neuroplasticity means that our thoughts, emotions, and our experiences (what we repeatedly sense, feel, and think) slowly sculpt the brain’s neural structure.
Neuroscientist Rick Hanson explains that rumination – getting caught in the same negative thought patterns – deepens the neural pathways and results in habitual negative thinking, which in turn causes persistent negative mood (8). Our persistent mental states become neural traits.
In other words, the more we felt depressed in the past, the more likely we are to feel depressed in the future.
Negative neural pathways not only impact our future ability to regulate our mood, they can affect our sleep patterns, memory, hormones and our immune system. They can lead to a negative spiralling effect that becomes increasingly harder to change over time.
Our brain’s neural structure changes continuously throughout our lives. Our thoughts create neural pathways like water creates a river. So, by redirecting our thoughts, we can remap our neural structure in positive ways, no matter how old we are.
FIND OUT MORE: How Monkey Therapy Helps You Alleviate Depression, The Science Behind Depression, Steps You Can Take Now to Alleviate Depression, Feeling Down but Not Clinically Depressed
References and Contributors
-
David Shariatmadari. (2015). What is depression? You asked Google – here’s the answer. The Guardian.
-
Center for Disease Control. (2012). Estimated 1 in 10 U.S. Adults Report Depression.
-
Robert Plutchik. (1980). Theories of Emotion (Volume 1).
-
Harvard Health Publications. (2009). Harvard Medical School. What causes depression?
-
Dan Siegel. (2010). Mindsight: The New Science of Personal Transformation.
-
Daniel Nettle. (2003). Review Evolutionary origins of depression: a review and reformulation.
-
Jed Diamond. (2014). The Irritable Male Syndrome: Understanding and Managing the 4 Key Causes of Depression and Aggression.
-
Rick Hanson. (2013). Hardwiring Happiness. The New Brain Science of Contentment, Calm and Confidence.
-
Bessel van der Kolk. (2014). The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma.
-
Karla McLaren. (2013). The Art of Empathy: A Complete Guide to Life’s Most Essential Skill
-
Daniel Goleman. (1996). Emotional Intelligence.
-
Helpguide.org, WebMD.org
How therapy works
Worksheets and useful information
Creative Process
Feeling Stuck
Stress
Depression
Feeling Down
Anxiety
Guilt and shame
Find out more
What I do differently
Monkey Therapy
Transformational Coaching
Online Therapy
Trauma
Your inner critic
The science behind it
Steps you can take now
Publications
More than CBT
More than IFS
Psychedelics
Neurodiversity
Thank you!
Your message has been sent. We'll contact you shortly
© 2023 The Monkey Therapist. All Rights Reserved. Site Designed By Samantha Ósk
PRIVACY POLICY